Thyroid Cancer | Vibepedia
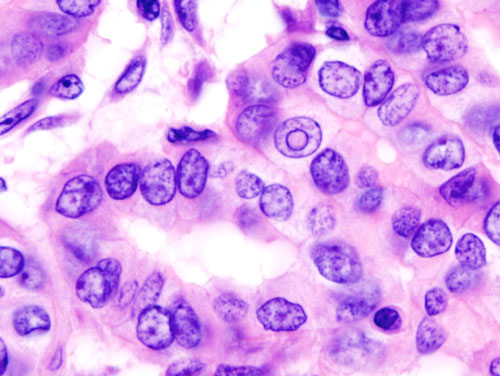
Thyroid cancer originates in the thyroid gland, a butterfly-shaped endocrine organ nestled in the neck. This disease is characterized by the abnormal…
Contents
Overview
Thyroid cancer originates in the thyroid gland, a butterfly-shaped endocrine organ nestled in the neck. This disease is characterized by the abnormal proliferation of thyroid cells. While often asymptomatic, symptoms can manifest as a palpable neck mass, voice changes, or difficulty swallowing. The incidence of thyroid cancer has seen a significant global rise, particularly in the last few decades. Diagnosis typically relies on imaging techniques like ultrasound and fine-needle aspiration biopsy. Despite its increasing prevalence, treatment often involves surgery, radioactive iodine therapy, and sometimes external beam radiation or chemotherapy. However, rarer, more aggressive forms like anaplastic thyroid cancer present formidable challenges.
🎵 Origins & History
The recognition of thyroid abnormalities dates back to ancient times. The understanding of thyroid cancer as a distinct entity is more recent. Theodore Kocher was a pioneering surgeon in thyroid surgery, laying the groundwork for thyroid surgery in the late 19th century. The discovery of radioactive iodine (I-131) revolutionized the treatment of differentiated thyroid cancers, offering a targeted therapy for metastatic disease.
⚙️ How It Works
Thyroid cancer arises from the uncontrolled growth of cells within the thyroid gland, which produces hormones regulating metabolism. These abnormal cells can originate from the follicular cells, which produce thyroid hormones, or the parafollicular (C) cells, which produce calcitonin. Papillary and follicular thyroid cancers are collectively known as differentiated thyroid cancers. These tend to grow slowly and are often treatable. Medullary thyroid cancer originates from C cells and can be hereditary, linked to mutations in the [[RET proto-oncogene|RET gene]]. Anaplastic thyroid cancer, the least common but most aggressive type, also arises from follicular cells but has lost most of its normal thyroid cell characteristics, leading to rapid growth and widespread metastasis. Diagnosis involves imaging like [[ultrasound|ultrasound]] and [[fine-needle aspiration|fine-needle aspiration (FNA)]] biopsy to examine suspicious nodules for cancerous cells.
📊 Key Facts & Numbers
Globally, thyroid cancer incidence has surged by over 200% in the past three decades, reaching an estimated 586,000 new cases in 2020, according to the [[world-health-organization|World Health Organization]]. The majority of these are differentiated thyroid cancers, with papillary thyroid carcinoma accounting for approximately 80% of all cases. The incidence is significantly higher in women than men, with a female-to-male ratio of roughly 3:1. While the overall mortality rate remains low at around 0.5 per 100,000 people annually, the dramatic increase in diagnosis, particularly of small papillary cancers, has led to debate about overdiagnosis. For instance, in South Korea, a screening program initiated in the 1990s led to a more than 15-fold increase in thyroid cancer diagnoses by 2011, with most being small, indolent tumors.
👥 Key People & Organizations
Pioneering surgeons like [[theodore-kocher|Theodore Kocher]] laid the groundwork for thyroid surgery in the late 19th century. In the mid-20th century, [[beverly-collen-robins|Beverly Collen-Robins]] and colleagues at the [[massachusetts-general-hospital|Massachusetts General Hospital]] were instrumental in developing radioactive iodine therapy protocols. More recently, researchers like [[steven-paschold|Steven Paschold]] at the [[university-of-pittsburgh-medical-center|University of Pittsburgh Medical Center]] have focused on understanding the molecular drivers of thyroid cancer, particularly anaplastic subtypes. Organizations such as the [[american-thyroid-association|American Thyroid Association (ATA)]] and the [[thyroid-cancer-society|Thyroid Cancer Society]] play crucial roles in patient advocacy, research funding, and disseminating clinical guidelines. The [[national-cancer-institute|National Cancer Institute (NCI)]] in the United States also funds extensive research into thyroid cancer prevention, diagnosis, and treatment.
🌍 Cultural Impact & Influence
The dramatic rise in thyroid cancer diagnoses, particularly in countries with widespread screening programs like South Korea and the United States, has sparked considerable public and medical discussion. This surge has led to increased awareness of the thyroid gland and its potential for malignancy, influencing public health campaigns and patient education initiatives. The phenomenon has also been explored in popular culture, sometimes highlighting the emotional toll of diagnosis and treatment, while also underscoring the generally positive outcomes for many patients. The visual representation of the thyroid gland, often depicted as a butterfly, has become a recognizable symbol for awareness campaigns, appearing on merchandise and in media to signify solidarity and support for those affected by the disease.
⚡ Current State & Latest Developments
As of 2024, the global landscape of thyroid cancer management is evolving rapidly. Advances in molecular diagnostics are enabling more precise classification of tumors and the identification of targeted therapies. For instance, drugs like [[dabrafenib|dabrafenib]] and [[trametinib|trametinib]] have shown efficacy in treating anaplastic thyroid cancers with BRAF mutations. Furthermore, research into [[liquid-biopsy|liquid biopsies]] is progressing, aiming to detect cancer DNA in blood samples, which could revolutionize early detection and monitoring of recurrence. The [[food-and-drug-administration|FDA]] continues to approve new treatments for advanced or refractory thyroid cancers, offering hope to patients with limited options. Ongoing clinical trials are exploring novel immunotherapies and combination treatments to improve outcomes for aggressive subtypes.
🤔 Controversies & Debates
A significant controversy surrounds the dramatic increase in thyroid cancer incidence, particularly the diagnosis of small papillary thyroid microcarcinomas (PTMCs). Critics argue that widespread ultrasound screening, especially in countries like South Korea, has led to overdiagnosis and overtreatment of indolent cancers that would never have caused harm or symptoms during a patient's lifetime. This debate, often termed the 'epidemic of thyroid cancer,' questions the benefit of aggressive screening versus the harms of unnecessary surgery, radiation exposure, and lifelong thyroid hormone replacement therapy. Another debate centers on the optimal management of indeterminate thyroid nodules, where FNA results are inconclusive, leading to varied clinical approaches and patient anxiety.
🔮 Future Outlook & Predictions
The future of thyroid cancer management points towards increasingly personalized medicine. Genomic sequencing of tumors will likely guide treatment decisions, with targeted therapies becoming standard for specific molecular subtypes. The development of more effective treatments for advanced and anaplastic thyroid cancers remains a priority, with ongoing research into novel drug combinations and [[immunotherapy|immunotherapy]] approaches. Furthermore, advancements in [[artificial-intelligence|artificial intelligence]] may enhance diagnostic accuracy in interpreting ultrasound images and pathology slides, potentially reducing diagnostic errors and improving efficiency. Efforts to better understand and mitigate the long-term side effects of treatment, such as cardiovascular issues and secondary malignancies, will also be crucial.
💡 Practical Applications
The primary application of understanding thyroid cancer lies in its diagnosis and treatment. For patients, this means undergoing diagnostic procedures like [[ultrasound|ultrasound]] and [[fine-needle aspiration|fine-needle aspiration (FNA)]] biopsy to identify suspicious nodules. Treatment options are tailored to the type and stage of cancer, commonly involving surgical removal of the thyroid gland (thyroidectomy), often followed by radioactive iodine (RAI) therapy to eliminate any remaining cancer cells. For differentiated thyroid cancers, RAI therapy is a cornerstone, utilizing the thyroid's natural uptake of iodine. External beam radiation therapy may be used for more advanced cases or those not responsive to RAI. Chemotherapy is typically reserved for aggressive, metastatic, or anaplastic thyroid cancers where other treatments have failed. [[Thyroid hormone replacement therapy|Thyroid hormone replacement therapy]] is essential after total thyroidectomy to maintain normal metabolic function and suppress TSH, which can stimulate residual cancer growth.
Key Facts
- Category
- science
- Type
- topic